Understanding the Function in Functional Neurological Disorder (FND)

When we talk about Functional Neurological Disorder (FND), we need to start with the word “function.” The symptoms that our clients experience aren’t random. They serve a purpose, even if it’s not within the conscious awareness of the client or the clinician. FND is a somatoform condition, meaning the body is expressing something the mind might not fully be able to express. These symptoms are a form of dissociation that show up in the body.
Reunifying the Body and Mind
One of the things that makes FND so complex is that it is neither purely mental nor purely physical. It sits at the intersection of the two and reminds us that the body and mind are something that cannot be separated. Oftentimes, the challenge is that research on FND and PNES is often rooted in neurology journals, focusing on medical perspectives. Meanwhile, mental health research lags behind. Within the mental health field, Cognitive Behavioral Therapy (CBT) is often recognized as the gold standard for treatment of FND and PNES. It is often the first and only form of treatment recommended for people with FND or PNES. While CBT can help, it doesn’t always address the deeper layers—particularly psychological and somatic dissociation. By nature, CBT focuses on cognitive understanding, processing, and conceptualization of the symptoms. However, FND symptoms often come from subconscious triggers and conflicts. CBT techniques can be helpful in the beginning to teach the client about various things such as the Cognitive Triangle-connecting the mind, body, and emotions. However, it provides little opportunity to help clients uncover and work through subconscious triggers and conflicts that both may be occurring internally or externally for the client.
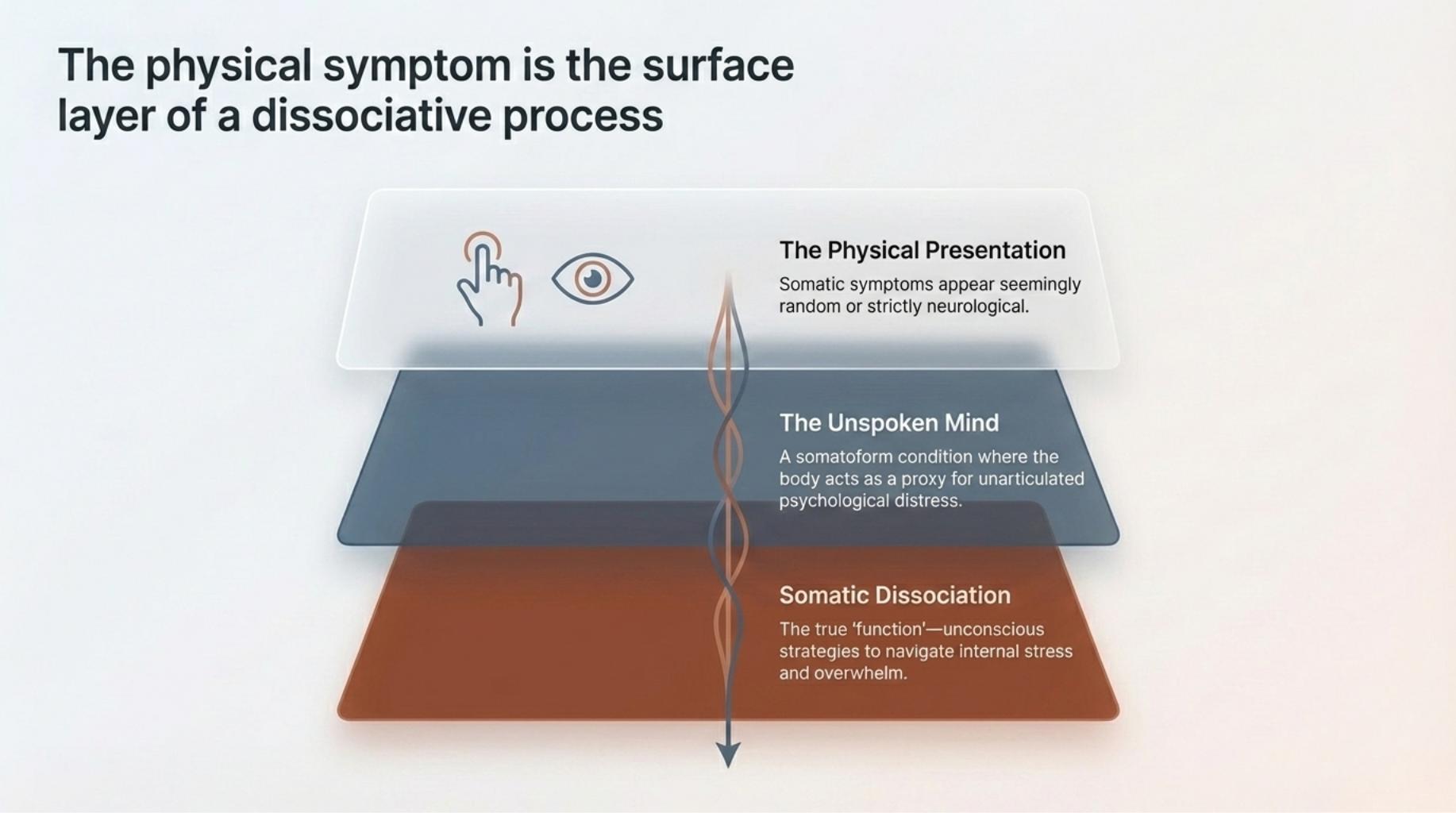
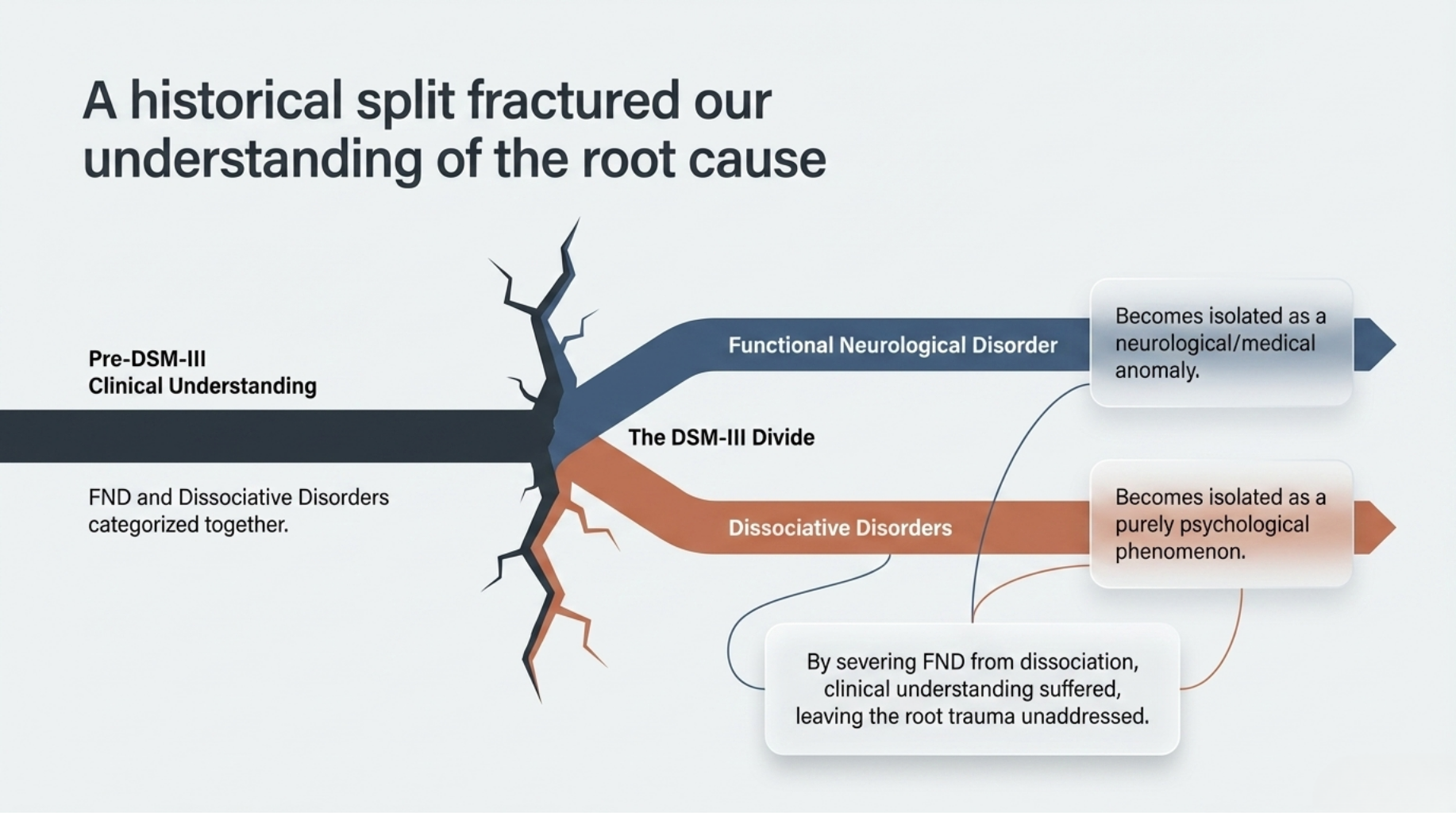
In order to reconceptualize FND and PNES, we need to reunify the separation between the body and mind. FND actually used to be categorized with dissociative disorders before the DSM-III separated them. Often times people with FND and PNES exhibit symptoms of psychoform dissociation. These types of dissociation include disruptions in memory, identity, conscious, and symptoms like derealization and depersonalization. When we look deeper at the somatic forms of dissociation, symptoms like psychogenic seizures, temporary paralysis, numbness, choking, or even temporary blindness serve a functional role for the client and often act as nonverbal, subconscious forms of communication within the psyche and body.
Symptoms of Communication
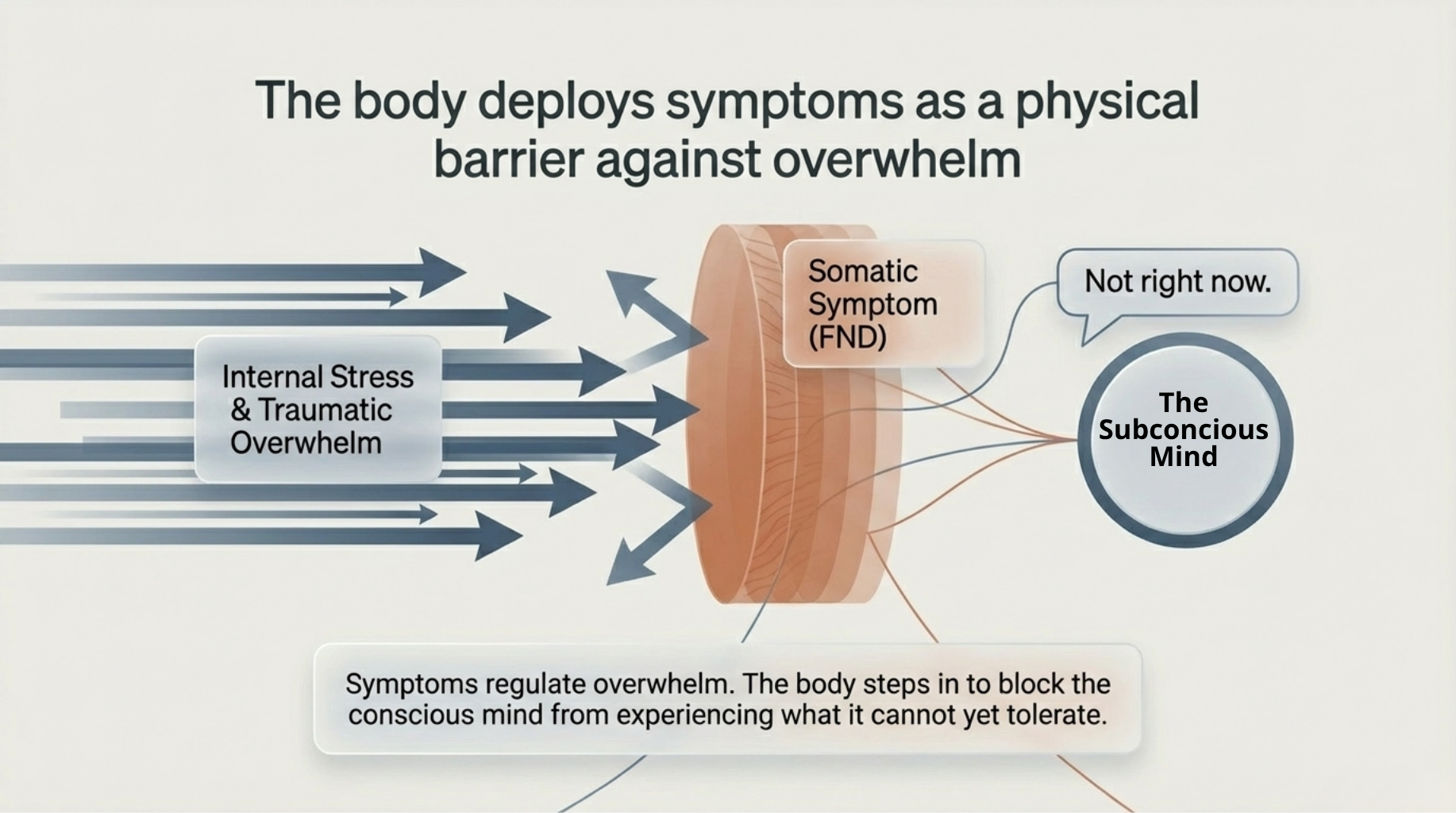
These symptoms can be a way for different self-states or ego states to communicate with each other. They may be regulating overwhelm or protecting the client. These symptoms can block the individual from seeing, hearing, or doing things that feel like too much or too overwhelming. It’s as though the body steps in to say, “Not right now.” However, long-term, the client needs to expand their tolerance for internal and external triggers and gradually face experiences in safe and manageable ways.
Symptoms of Remembering
Sometimes, what looks like a purely physical symptom on the surface, such as sudden numbness or loss of sight can actually be a somatic flashback. In other words, the body is re-experiencing a dissociated element of past trauma, but instead of a clear conscious memory, it’s showing up as a physical sensation or loss of function. This is why FND can be so complex—because you’re dealing with layers of dissociation, and sometimes, the body is holding pieces of the trauma that the mind hasn’t fully integrated. By understanding that these symptoms can be somatic flashbacks, we’re better equipped to help clients not just manage the symptoms, but process the underlying trauma safely. In doing so, we must conceptualize the client's experience in a more holistic approach and ensure to develop a treatment plan that will support integrative processing of all elements of the trauma. This must be accomplished in a safe way, allowing the client to integrate and process all aspects of the memory without flooding or worsening of FND symptoms.

Understand, Expand, Integrate
So, the function in FND is this: these symptoms are strategies—albeit unconscious ones—to navigate internal stress and overwhelm. To help our clients, we need to address not only the symptom but the underlying dissociative processes—both psychological and somatic. FND isn’t just something to manage; it’s something to understand deeply, so we can help the client find safer, more adaptive ways to function. By utilizing a deeper, more holistic approach, we are able to help our clients navigate to deeper layers of understanding or their triggers, traumas, internal conflicts, and internal needs.
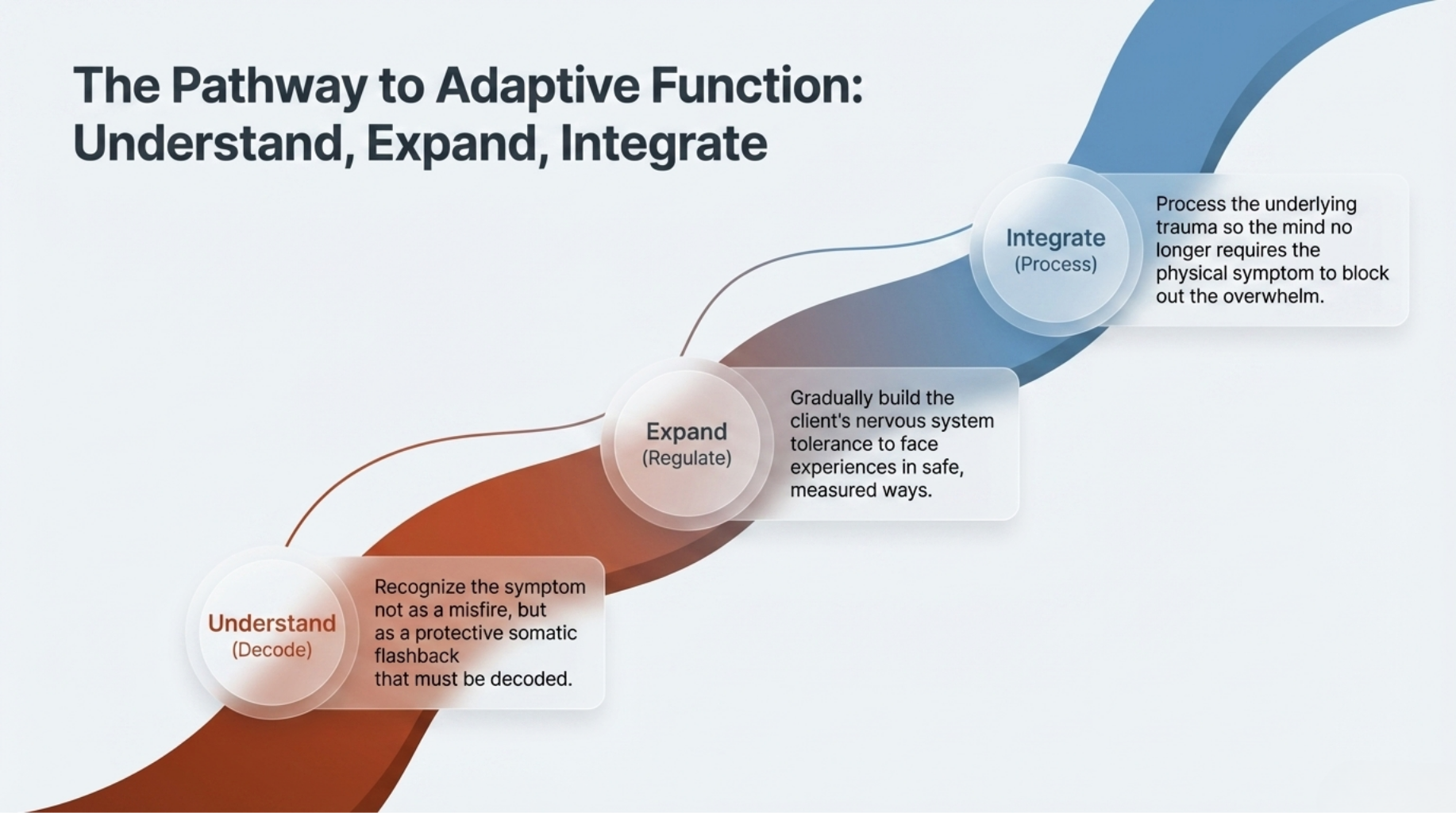
Ultimately, when we begin to view FND through this lens, the work shifts. We move away from trying to eliminate or suppress symptoms and toward understanding what they are communicating. This doesn’t mean the symptoms are intentional, but it does mean they are meaningful.
As clinicians, our role is to help clients safely build awareness, increase tolerance for internal experience, and gently reconnect the parts of themselves that have been divided through dissociation. This requires patience, attunement, and a willingness to move beyond purely cognitive approaches into deeper, integrative work.
When we approach FND in this way, we are no longer just treating symptoms—we are helping clients restore connection within themselves. And in that reconnection, there is not only symptom relief, but the potential for lasting healing.
Phoenix Arise Consulting

